Insulin is life for those of us living with T1D and many of those with other types of diabetes. There are many nuances to taking insulin, including the importance of rotating where insulin is injected into the body. When insulin is injected repeatedly in the same part of the body, it can cause changes in the skin that make insulin absorb erratically. Here’s some more information to help you avoid unnecessary challenges with managing blood sugars.
Lipodystrophy
Anyone who took Latin or medical terminology classes, this will be a little easier for you! For the rest of us, we’ll break down the meaning – “Lipo” means “relating to fat” and “dystrophy” literally means “bad nutrition,” but generally refers to a disorder that negatively affects the tissues of the body. So basically, Lipodystrophy means changes to the fatty tissue where insulin is normally injected or infused.
There are two main types of Lipodystrophy: Lipoatrophy and Lipohypertrophy. Lipoatrophy is when there the tissue atrophies or wastes away. The opposite is Lipohypertrophy, where the tissue gets bigger, typically forming hard lumps of what is commonly referred to as scar tissue. Both are common, and although Lipohypertrophy tends to be more common, both can negatively affect glucose management.
How do you spot it?
Sometimes it’s very easy to spot skin changes from insulin, and sometimes it’s more difficult. A recent study looked at 316 people with diabetes who continuously used insulin for a year, and 19.9% had what they called subclinical lipohypertrophy.1 This meant that it couldn’t be seen or even felt by the provider, but when doing an ultrasound, it became obvious that there were changes in the tissue.1
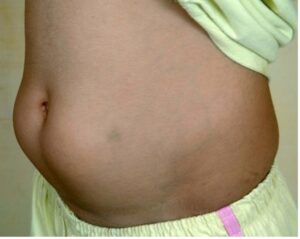

Other times, the changes in skin are very visible, such as the example below from the BMU Case Reports in 2017. Although it’s not always this pronounced, it can usually be detected by feeling the tissue in the areas where insulin is injected or infused. If your diabetes healthcare team is not examining and feeling the skin where you take your insulin, you should ask them to do so. You can also try feeling your own skin, and if you notice any hard nodules, try to avoid them until they heal.
How common are skin issues for people with diabetes?
There is not enough data to determine how common skin issues are for people with diabetes, but if you look in many online social media platforms that have diabetes groups, you’ll likely see questions about skin issues. Often people ask about allergies to adhesives, inability to keep adhesives on, or possible infections. It’s rare for people to talk about lipodystrophies, possibly because people are not familiar with this as a complication from taking insulin, or because they feel ashamed to talk about it.
In a study from 2020, 91.8% of the 369 participants had signs of diabetes-related skin conditions, 45.8% of whom had lipohypertrophy.2 In this study, 46.8% of those with lipohypertrophy used an insulin pump and 43.1% were on multiple daily injections, meaning it was only slightly more common when on an insulin pump. As far as lipoatrophy, only 2.7% of the 369 participants showed evidence of the condition.
This study also looked at various rashes, skin infections, and skin disorders for people with diabetes, and it showed the possible impact that diabetes has on the skin in many ways. For example, 37.5% of participants had something called Keratosis Pilaris, which is where the skin produces too much keratin and it causes a raised red bumpy rash. Ironically, this is something I believe I have on the back of my arms, likely due to my CGM placement, and had never heard of until writing this article.
What is the treatment?
When it comes to lipohypertrophy and lipoatrophy, the treatment is simple – you must avoid using the tissue for 6-12 months, depending on the severity. This sounds easy enough, but if you are lean or have a lot of tissue affected, it can be difficult. It’s also not always the most comfortable to try new locations for injections or infusion sets. Personally, I have tried to use my thighs on occasion, and cannot seem to feel comfortable or avoid accidentally ripping the infusion set off.
For rashes or infections, asking your healthcare team is your best bet. If your skin is warm to the touch, raised, red, painful, or oozing any fluid, it may be an infection. Some infections will require topical creams, while others may need oral antibiotics. Although infections were less common in the studies, they do happen, and are more likely to happen if your blood sugars are running high. The bacteria love that extra sugar.
Insulin injection and infusion rotation
To help prevent lipodystrophies, rotate the places you inject or infuse insulin in a pattern. Many people will go back and forth from their left to right side of the body and inevitably choose the same places. To avoid this, many diabetes education and care specialists, including myself, will recommend picking some sort of rotational pattern. Some people use letters such as “W” or “M”, others use the “planting the seed method” where you inject about a half inch away from the last injection site.
Personally, I use my left side of my body for one month and the other side the next month. As an example, for September this year I’m using the right side of my body. This allows me to give the other side of my body about 30 days of rest from insulin infusion. I’ve been using an insulin pump for 22 years now, so I need to be cautious about overusing my favorite spots. You can put insulin into any part of your body that has fatty tissue, or anywhere you can “pinch an inch.” See diagram below.


A couple of weeks ago, I was experiencing some erratic blood sugars, more erratic than the usual ups and downs of diabetes. I couldn’t figure out what was happening because I couldn’t necessarily feel any lumps of scar tissue, but once I switched to another part of my body, my blood sugars were less chaotic. As a result, I’m letting that part of my body rest for the next couple of months.
At the end of the day, I know I’m going to have high blood sugars, but I want them to be for good reasons. Such as having eaten a delicious cookie that I didn’t carb count correctly. What I don’t want are annoying high blood sugars because my insulin didn’t get absorbed in my body properly. So, I keep on rotating, and I hope this helps you rotate your insulin sites as well.
- Subclinical lipohypertrophy–Easily ignored complications of insulin therapy
- Pediatric diabetes and skin disease (PeDiSkin): A cross-sectional study in 369. Children, adolescents and young adults with type 1 diabetes
Written and clinically reviewed by Marissa Town, RN, BSN, CDCES



