Shaping Expectations at Diagnosis
I feel very fortunate to not have much memory of my diagnosis. I was only 2 years old, and the only memories I have include a vague vision of a hospital room and my experience talking to my first diabetes psychologist. The diabetes psychologist memory is more vivid, and I remember coloring in a large room at a little toddler sized table and chair while a lady asked me questions. I remember thinking, “Why is she asking me questions? All I want to do is color.”
What I do know about my family’s diagnosis experience I’ve heard from my parents, and from hearing about many others’ diagnosis experiences, I know we were very lucky. First, I was not in DKA and didn’t have a long intensive care stay. Second, the child in the bed next to mine when I was in the hospital had Cystic Fibrosis, which is a very severe illness in the lungs that at the time in 1989 had a bleak prognosis. And third, the endocrinologist told my parents that I was going to be okay, and I could live a normal life
These experiences helped my parents understand that although their lives and mine would be forever changed, it was not the worst thing that could have happened. They knew they would have to work hard to learn all there was to know about diabetes to help keep me safe, and that they would work together as a team with the endocrinologists, diabetes psychologists, and diabetes educators to help me live as normal of a life as I could.
Fingersticks and Logbooks
For those of you newer to diabetes back then, (wow, I’m getting old…) we did not have continuous glucose monitors (CGMs). In fact, in many places of the world people still do not have access to this transformative technology. So, what did we do? Were my parents any less anxious about knowing what my blood sugar was doing at every waking and sleeping moment? Probably not, but there was not a way to keep watch like we can with CGM.
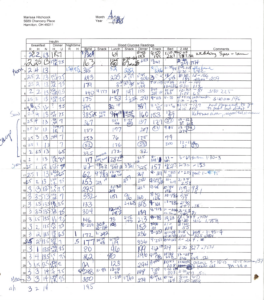

Many well-meaning healthcare professionals ask people with diabetes to keep logs as a way of identifying glucose patterns and helping figure out where adjustments can be made to keep levels closer to targets. As you can imagine, or know from experience, keeping a log is a royal pain in the behind. I had the unfortunate experience of being required to log for my entire pregnancy (my son is almost 10, so hopefully this doesn’t happen to anyone anymore…if it is, let me know who to call 😉).
The reality of diabetes is shown in these logbooks – there are highs, there are lows, and sometimes you get close to your goals. Not shown is all of the hard work that goes into getting to goal and the emotional weight of it all. The pregnancy log shows how healthcare professionals sometimes use logbooks. They circle numbers that are out of target to identify what needs adjusted.
If you ever want to make a pregnant woman with diabetes mad, circle blood sugars that are close to target. See glucose level of 92 for before dinner when the target is 50 to 90 mg/dl. Also, can we just take a second to talk about how log 50 mg/dl is? Thankfully, the guidelines for pregnancy changed a couple years after my son was born, relaxing the stringent guidelines for women with T1D. As you can see, there are a lot of serious lows on there, including a 31 mg/dl at 3 a.m. one night. Not ideal, but we made it through the whole thing. (See article about pregnancy here)
The other reality of logbooks is most people will not do them. Why? Because it’s ridiculously annoying and time-consuming to do it. During pregnancy it felt a little bit more of a reasonable request because my fetus was depending on me for life, but even then I was very frustrated to have to do it. And checking blood sugars often enough to collect meaningful data can be difficult.
Realities of CGM
Even if you’re fortunate enough to have access to a CGM, it’s not without its challenges and flaws. Many people struggle with alarm fatigue and stop paying attention to their CGM alerts. Others have heightened anxieties about blood sugars – some high, some low, some are anxious about all of it.
Having real-time access to changes in glucose levels is a new phenomenon and people with diabetes and their families don’t always have the right resources or training in how to deal with this newfound data stream. Additionally, there are many people experiencing skin issues related to wearing devices on their bodies constantly. Some find that their devices aren’t staying stuck on long enough, while others develop severe allergies to the tapes.
How we talk about CGM also really matters. At every Friends for Life conference, we hear over and over from kids with T1D how frustrated they are with their parents watching their every glucose level every 5 minutes. In clinic, we have parents asking why their child’s CGM is not working and the solution all too often is that someone is closing out the CGM app. Whether or not this was accidental is unclear, but kids are smart and they know how to use devices better than their caregiver(s).
It’s so easy for parents to get worked up over their child’s glucose levels and even assume that they made a poor choice that caused the changes in levels. This comes from a place of love and concern – which is such a beautiful thing to have. So why not talk to your child to see how they want to talk about their CGM values/trends/etc.? Everyone is different, and what works for one person may not work for someone else.
This same thing applies to adult support systems – friends, partners, coworkers, fiffles (short for Friends for Life, AKA FFLs), other relatives, etc. For me, my spouse has always been my follower, among others usually for demonstrative purposes; but he is my key diabetes support system. Since we are partners it means that the conversations are on a level playing field, which is a very different dynamic than parent and child. But both scenarios require clear, honest communication.
Here are my key recommendations for CGM Communication (also probably applicable to other areas of diabetes management):
- For the person with diabetes – SPEAK UP!
- Don’t wait until you’re already super frustrated.
- Remember, you don’t want to do this all alone, support is important!
- For a parent – focus on the behavior NOT the outcome!
- Diabetes fails me every single day, and I am a diabetes educator and a nurse literally trained to do diabetes. It’s impossible to get it right; cut us some slack.
- If you provide your child with a phone to use their CGM and share data with you, your rules need to be followed.
- Whether this is keeping CGM on most days of the week, not closing the app, telling your parent if you’re having CGM issues, etc.
- For an adult support person (And the world!)– please don’t judge us! (see 2a)
- We put a lot of pressure on ourselves as PWD, we feel it from our doctors, our nurses, our parents, our pharmacist, our nosy neighbors and random relatives, we know when we muck things up, so just be there for us, ok?
- Ask your person with diabetes how they want you to talk about their numbers or trends or if they want you to talk about it all.
- My husband has learned that he gets the best response from me when he says, “BG my beautiful?” or “Are you aware of your blood sugar? This way I feel both supported and beautiful 😊
- This is also very applicable to parents – talk to your kiddo and see if they want you to use emojis or GIFs versus text or –GASP– a phone call. I highly recommend incorporating some levity and humor when you can, and emojis and GIFs are a language the youths seem to understand. If you need help navigating these conversations, ask your diabetes team for help! Hopefully they will have a diabetes psychologist or a social worker who may be able to help.
- My husband has learned that he gets the best response from me when he says, “BG my beautiful?” or “Are you aware of your blood sugar? This way I feel both supported and beautiful 😊
- For All of Us – Celebrate the wins.
- It’s important to celebrate the times when you really knock it out of the park in some way in diabetes. It could be on purpose, could be complete luck, but either way – enjoy the moments!
- We have a friends with diabetes text group and send screenshots of both our struggles and our wins.
- My partner will occasionally screenshot a 100 with a flat arrow (3:00 on the clock) and say that he owes me a dollar. He never pays, but it’s the thought that counts.
- When you go to the doctor/nurse practitioner/see that random relative again show them that CGM graph and tell them you are rocking in! Or, send them a nice email showing your hard work.
- It’s important to celebrate the times when you really knock it out of the park in some way in diabetes. It could be on purpose, could be complete luck, but either way – enjoy the moments!
I hope this has helped validate some of your feelings related to diabetes and its many challenges and reminded you that you are not alone in this journey. Until there’s a cure, there’s CWD.
Written and clinically reviewed by Marissa Town, RN, BSN, CDCES



