Glucagon for Severe Hypoglycemia
Low blood sugars can be a scary part of life with diabetes, but being informed and prepared on how to treat hypoglycemia can make these moments less stressful. Glucagon is the best treatment option for severe hypoglycemia.
What is glucagon?
Glucagon is a hormone that raises the level of glucose in the blood. The alpha cells of the pancreas, in areas called the islets of Langerhans, make glucagon when the body needs to put more sugar into the blood. Glucagon binds to a receptor on liver and muscle cells (called the glucagon receptor), stimulating the cells to release glucose.
For people with type 1 diabetes, the pancreas does not release insulin, making them unable to adjust insulin levels in response to glucose levels, and type 1 diabetes can also impede the secretion of glucagon, making them at risk for severe low blood sugars.
Everyone who uses insulin should have a form of glucagon on hand at all times to counteract severe hypoglycemia that causes loss of consciousness, or if sugar cannot be given. See below for the kinds of glucagon that are available.
One of the potential side effects of a rescue dose of glucagon -- regardless of the form -- is vomiting, so be sure to place the person on his or her side prior to administering so they do not choke. After administering glucagon, follow with food once the person regains consciousness and is able to swallow.
Modern Glucagon Products
Families with type 1 diabetes have more choices than ever for glucagon products. These modern glucagon products are much easier to use than the old emergency glucagon kit. Discuss with your diabetes care team which of these is best for you.
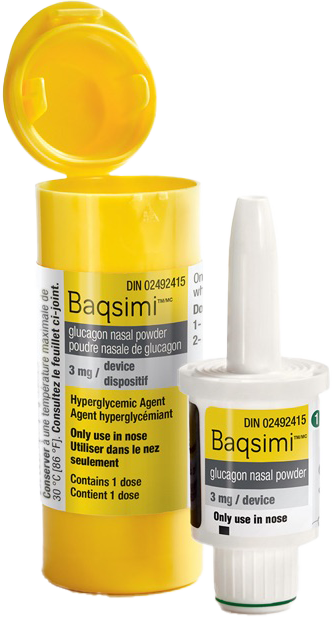
BAQSIMI Nasal Glucagon
BAQSIMI, made by Eli Lilly, is the first and only dry nasal powder to treat severe hypoglycemia. Instead of an injection, BAQSIMI is administered as a puff in the nose. It is important to note that BAQSIMI can be given to a patient who unconscious, as it does not require being actively inhaled and can be used even if the patient has a congested nose.
Keep tube sealed until ready to use.
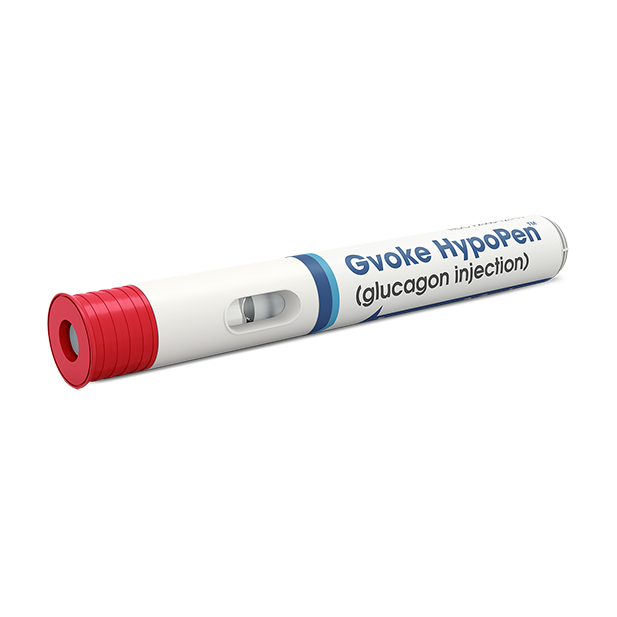

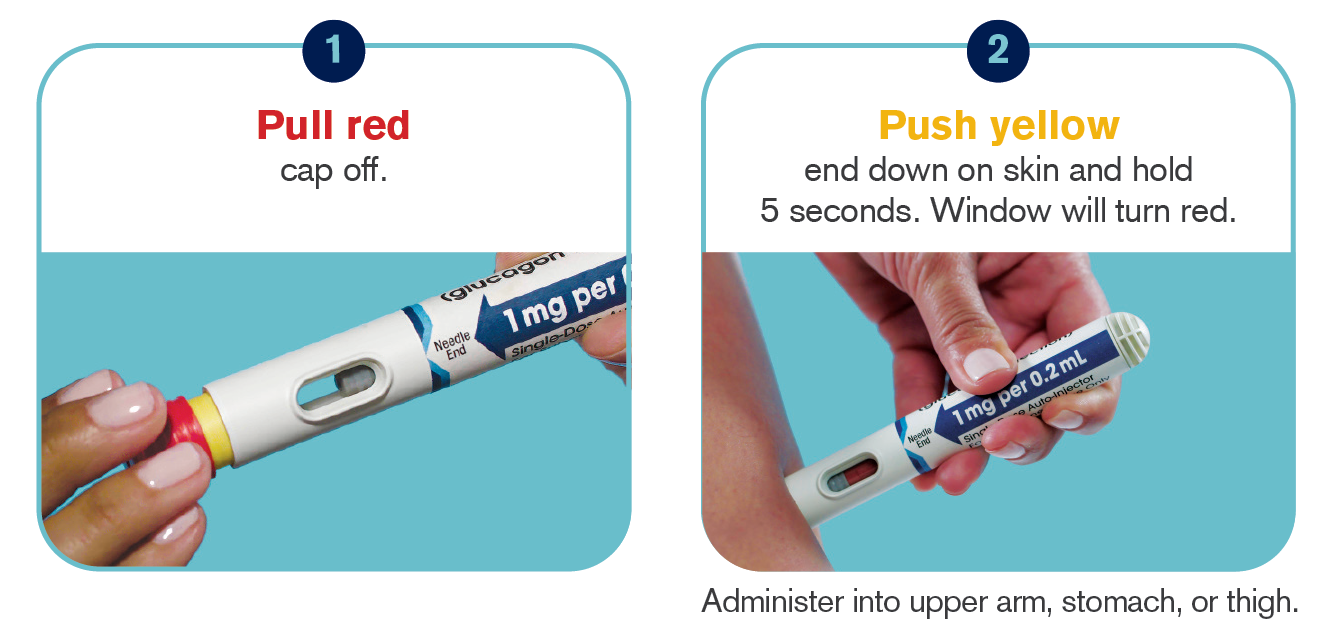
GVOKE HypoPen
The GVOKE HypoPen, made by Xeris Pharmaceuticals, is the first premixed autoinjector for very low blood sugar. GVOKE contains stable liquid glucagon and is available as a HypoPen and as a pre-filled syringe. Using the GVOKE HypoPen is an easy, two-step process, shown below.


Injectable Glucagon Emergency Rescue Kit
For years, families relied on the glucagon emergency kit to treat severe hypoglycemia. These kits, made by Eli Lilly and Novo Nordisk, included dried glucagon and a diluent and had to be mixed immediately before using. Due to the complicated nature of needing to mix this kit in an emergency situation, these glucagon kits can be challenging to use in the stressful situation of severe hypoglycemia. Studies have shown that people are much more likely to administer a rescue dose of glucagon using BAQSIMI or GVOKE compared with the old glucagon rescue kit. However, the “older” glucagon emergency kits can be used for mini-dose glucagon rescue.
Rescue kits of glucagon can also be used, in small doses, to raise blood sugar when someone can't eat -- for example, when sick due to a stomach illness. This is called mini-dose glucagon rescue, and while it is off label, many people with type 1 diabetes report using it with great success. Talk with your clinical team about how you or your family can use mini-dose glucagon with confidence.


Lilly's Glucagon Emergency Kit, opened. Lilly will no longer be making this kit as of December 31, 2022.
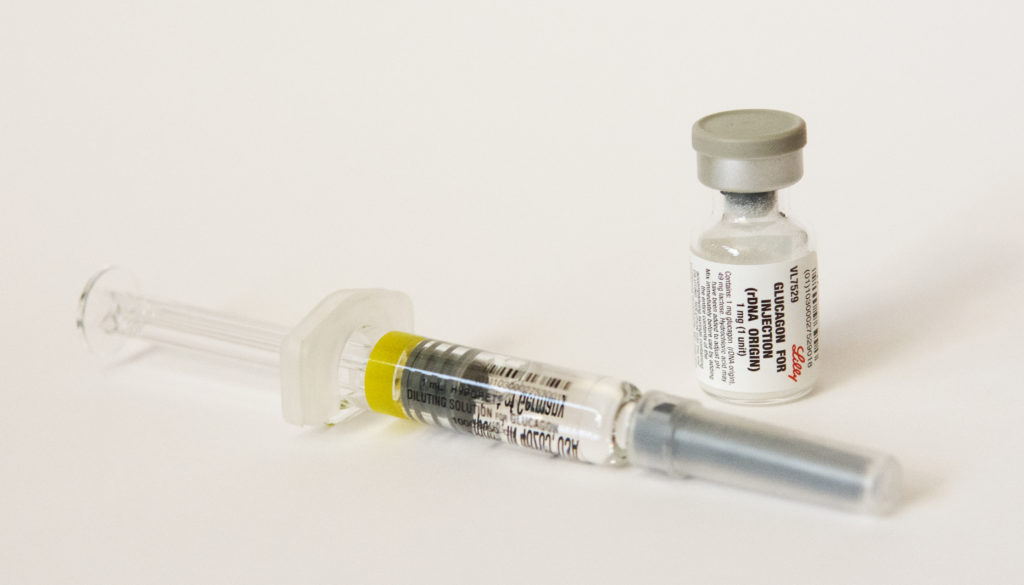

The syringe filled with diluent and the vial filled with the dry powder glucagon from the Lilly Glucagon Kit
- BAQSIMI dry nasal glucagon powder
- GVOKE HypoPen Pre-filled Pen
- Lilly Glucagon
- Novo Nordisk GlucaGen
- The Physiology of Glucagon from the NIH website
- What is Glucagon?
- The structures of receptors involved in blood sugar control
- Step-By-Step Guide to Using Glucagon
- A New Option for Emergency Hypoglycemia in Children?
- All About Glucagon
- Research Review: Glucagon Options, Hypoglycemia, and Emotions
- Glucagon Nasal Powder: A Promising Alternative to Intramuscular Glucagon in Youth With Type 1 Diabetes (HTML | PDF)
- Efficacy and Safety of Mini-Dose Glucagon for Treatment of Nonsevere Hypoglycemia in Adults With Type 1 Diabetes
- Comparative Pharmacokinetic/Pharmacodynamic Study of Liquid Stable Glucagon Versus Lyophilized Glucagon in Type 1 Diabetes Subjects
- Nonaqueous, Mini-Dose Glucagon for Treatment of Mild Hypoglycemia in Adults With Type 1 Diabetes: A Dose-Seeking Study (HTML | PDF)
- Development of a highly stable, nonaqueous glucagon formulation for delivery via infusion pump systems
- Preserved glucose response to low-dose glucagon after exercise in insulin-pump-treated individuals with type 1 diabetes: a randomised crossover study (HTML)
- Low doses of dasiglucagon consistently increase plasma glucose levels from hypoglycaemia and euglycaemia in people with type 1 diabetes mellitus (HTML)
- Faster Use and Fewer Failures with Needle-Free Nasal Glucagon Versus Injectable Glucagon in Severe Hypoglycemia Rescue: A Simulation Study
- Human factors studies of a prefilled syringe with stable liquid glucagon in a simulated severe hypoglycemia rescue situation
- Nasal Glucagon Delivery is More Successful Than Injectable Delivery: A Simulated Severe Hypoglycemia Rescue
- Glucagon Nasal Powder: A Promising Alternative to Intramuscular Glucagon in Youth With Type 1 Diabetes