Written and clinically reviewed by Marissa Town, RN, BSN, CDCES
My friends with diabetes and I often joke which came first, the type A personality tendencies or the type 1 diabetes? When you’re diagnosed with diabetes at a young age, it’s hard to say what pieces of your personality are attributed to growing up with a chronic condition and what is just your personality, regardless of health conditions.
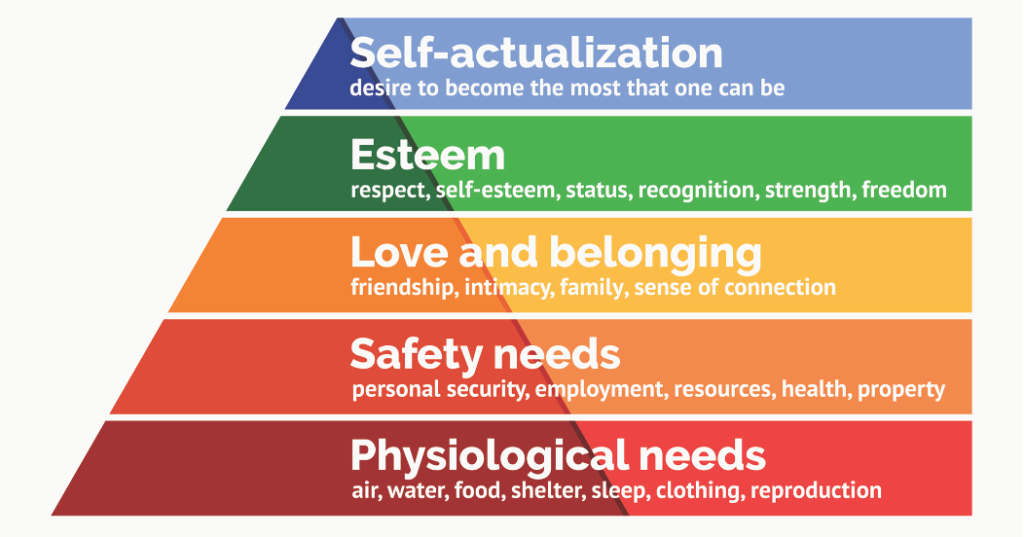
When I was in nursing school, I learned about Maslow’s Hierarchy of needs and realized that it made sense to me completely. How could my emotional needs be met if my body was in a constant struggle for its physiological balance? How could I feel calm when the blood glucose in my veins, that are in every part of my body, is too high or too low? And how could all of these things not affect who I become?

The other big piece of diabetes, aside from blood sugar data, is how other people treat you or talk to you about your diabetes. As authors in the article, “Diabetes Identity: A Mechanism of Social Change,” write: “The shame, blame, and stigma around diabetes intensified, and the attribution of poor diabetes control latched to willful characters instead of biophysical factors.” (Qualitative Health Research, 21 (5), 2021) This article goes on to discuss how the research around diabetes identity was focused on getting people with diabetes to do what they’re “supposed to do,” like check blood sugars, reach targets, live healthy lifestyles, etc.1
Drs. Heather Walker and Michelle Litchman decided they wanted to examine diabetes identity from the perspective of people living with diabetes, not through the lens of our health care teams. They interviewed twenty people with diabetes who are active in the Diabetes Online Community (DOC) and aimed to find out if being active in the DOC influences their sense of identity, what the components of diabetes identity are, and if counter-narratives affect diabetes identity.1 Many people who were interviewed felt that diabetes, “is a part of me, but is not all of me,” which has been a big theme of the messages in the DOC for some time now.1
The results of the interviews showed the following themes:
- Willingness to Identify (it’s a part of me, but is not all of me)
- Tales of the Un-Sick (to avoid being labeled as disabled or sick)
- Legends of the Responsible (needing to plan for possible BG excursions)
- A Tradition of Change-Making (helping others through your diabetes experience)
- Sense of Sameness (knowing people who really “get it”)
- Diabetes Identity as a Unifying Social Category (the difficulties we have as PWD that others do not such as navigating a healthcare system with extremely expensive out of pocket costs)
The article goes on to say, “The Findings of this study also point to the concept of control, which is a problematic concept…because…the physical, emotional, and mental ebb and flow of one’s physical glucose levels cannot be neatly detached from the social concept of control.” (Qualitative Health Research, 21 (5), 2021) Dr. Walker also states, “People with diabetes are trying to change the public perception of what it means to live with diabetes. People with diabetes want the world to know that being diabetic means being responsible, not lazy.”
The authors discuss a need to reach out to more marginalized people with diabetes and those that are not engaged in the DOC. But the research shows that many of us have similar feelings related to diabetes, and that many of us want to help make things better for all of us. Dr. Walker states, “Diabetes identity as a unified social group can be powerful, especially if we focus less on the splintering within our communities.”
Let’s continue to come together in the DOC, in person (hopefully soon!), and with our peers with all types of diabetes to help make our experiences with diabetes a little less challenging. Check out our upcoming events on our community page: cwd.is/community.

